The Yukon government and BC Renal Agency have signed a letter of intent to put in writing an already decades-long relationship that allows Yukoners with kidney disease to access at-home dialysis and other treatment.
In a press release March 4, the Yukon government described the signing of the letter as a “new partnership” and one that will “maximize opportunities for Yukoners to receive home hemodialysis in Yukon.”
However, in separate interviews March 5, both Dr. Adeera Levin, the executive director of the BC Renal Agency, and Karen Chan, the Yukon Department of Health and Social Services’ assistant deputy minister of corporate services, said little, if anything would change to the supports Yukoners with kidney disease already receive once an agreement is signed.
(The letter is just a precursor to an actual agreement on the provision of services to Yukoners with kidney disease. Neither Levin nor Chan could say when the agreement itself would be signed.)
“We’re basically formalizing what’s been a long-standing gentleperson’s agreement between the Yukon and BC Renal,” Levin said.
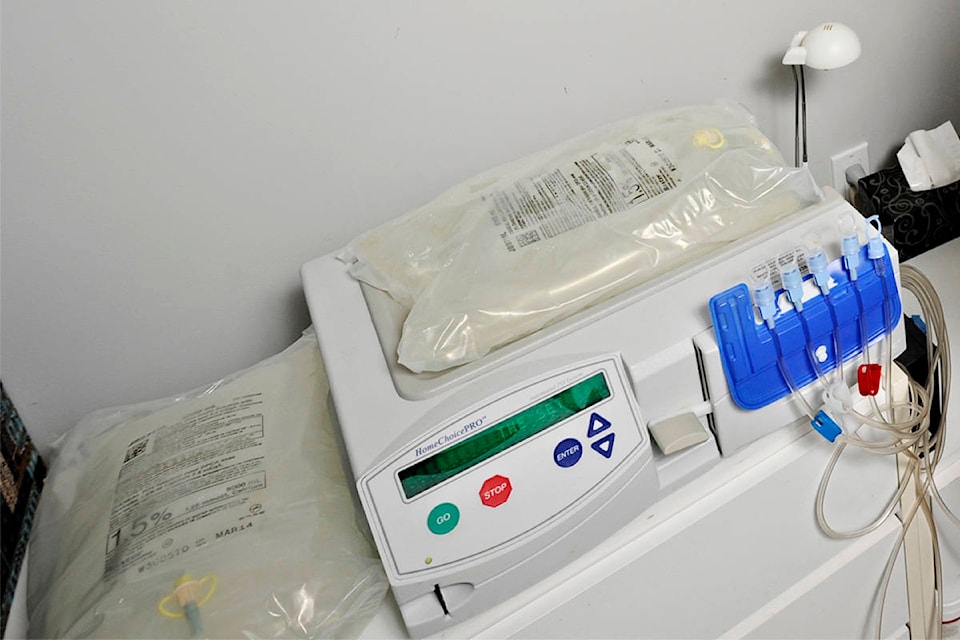
The BC Renal Agency, for the past 30 years, has accepted Yukon patients to its specialized clinic via physician referrals. Among the services Yukoners can access is a home dialysis program, where patients are provided with equipment, training and medical support to perform dialysis at home. Yukoners with end-stage kidney disease can also travel to British Columbia or Alberta for more specialized, in-hospital dialysis care or transplants.
That system has essentially been based on “goodwill,” Levin explained, in theory subject to the whim of various players on either side of the border. A formal agreement will ensure that Yukon patients will have access to services from the BC Renal Agency “independent of people’s good nature, if you will.”
“So it’s business as usual, with an added security that this will continue and be enhanced in perpetuity,” she said.
“… We have always been doing this and it’s been based on trust and a handshake, and sadly in the current world perhaps, it’s just really important that we have it more formal than that.”
Chan said that the agreement, once signed, will allow the Yukon to better evaluate and address the needs of Yukon patients and allow for greater focus on prevention efforts and early-stage kidney disease treatment.
Formalizing the system, she continued, is something the Yukon government has been researching and thinking about for years. She did not provide a clear explanation as to why it was happening now.
Both Levin and Chan said that implementing an in-hospital dialysis program in the Yukon is not a financially viable option, and not one the Yukon government is considering.
That topic came up most recent in late 2019, when Yukoner Terry Coventry, who required in-hospital hemodialysis to live, chose to return home to the Yukon rather than continue to receive treatment in Vancouver. The choice meant Coventry faced certain death, but he urged the Yukon government to bring the treatment to the territory for people who would come after him; he died in early January.
There are currently nine Yukoners on home peritoneal dialysis and none on home hemodialysis, according to Levin, emphasizing that the numbers often fluctuate due to people moving, dying or changing care systems.
Contact Jackie Hong at jackie.hong@yukon-news.com