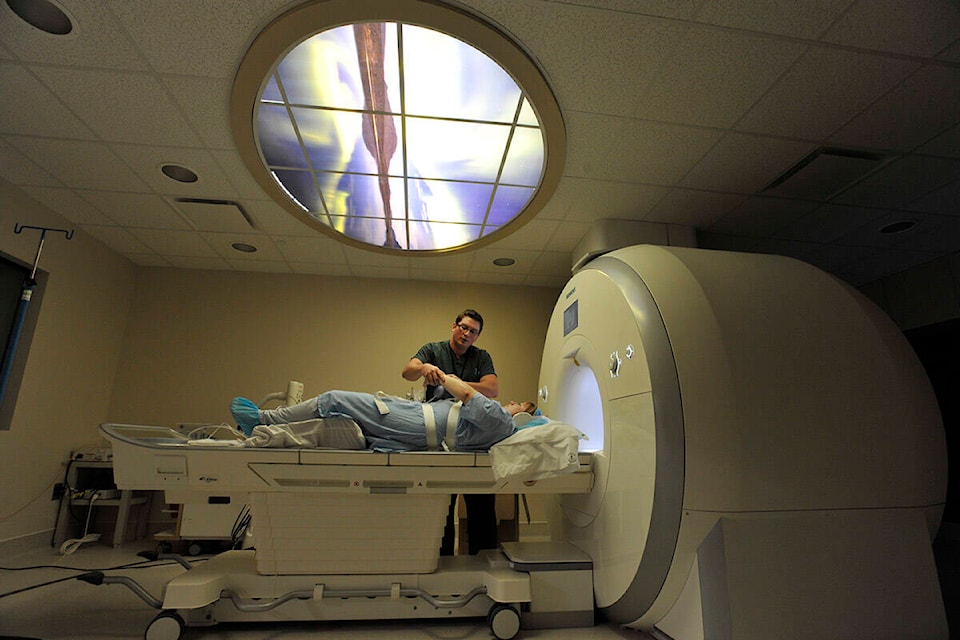
Health Minister Tracy-Anne McPhee says the current waitlist for non-urgent MRIs in the territory is around 1,000 people.
The issue of wait times for the hospital’s magnetic resonance imaging (MRI) machine was raised in the legislature March 28 by NDP leader Kate White. The MLA said people are waiting as long as nine months for a scan.
“A new MRI was supposed to make it easier for family doctors to refer patients for faster diagnosis, but with all the positive points came a negative one: wait times began to grow and grow,” said White.
An MRI is a non-invasive method of getting a better look at organs, tissues and skeletal systems that can be used to diagnose conditions where CT scans, X-rays or ultrasound are not suitable.
The Yukon is the only territory with the machine, after a Yukon Hospital Foundation fundraiser and government funding resulted in the machine beginning operation in 2015, but staffing it appears to be more difficult.
McPhee emphasized that wait times for urgent appointments are currently less than seven days. Semi-urgent appointments, which the hospital aims to get in close to 30 days, are now sitting around 44 days on average.
Non-urgent MRIs can wait up to 20 months.
Right now there is one full-time technician who is relieved during the year by locums. The backlog, she said, occurred during an unexpected vacancy in the position in December.
McPhee said the hospital corporation is currently trying to recruit more staff.
“The MRI program has been back on track and the Yukon Hospital Corporation is currently using a combination of local and casual technologists to ensure that acute and time-sensitive exams are completed in a timely manner,” she said.
Yukon Party leader Currie Dixon said he wants to see more funding provided to the hospital, while White said longer hours running the machine could help chip away at the backlog.
McPhee said the hospital corporation has plans to increase capacity.
“A single MRI technologist can handle between about 2,220 to 2,500 patients per year. That has been working well. But we know that the population of Yukon is expanding. So the need now is closer to 3,000 patients annually. So we’re going to need to make sure that there is capacity,” she said.
McPhee said medical professionals have the option to send patients down to Vancouver if an urgent need can’t be accommodated in the Yukon.
But White said that isn’t good enough.
She shared the story of an individual who has been waiting nine months for an MRI while dealing with daily symptoms. In another case, a person decided to go to a private medical clinic in Vancouver at a cost of $3,500 rather than wait for an appointment in the territory.
“Forcing people toward private clinics for a diagnosis that they should be able to access in the Yukon is unacceptable,” argued White.
McPhee noted that the designation of urgent, semi-urgent and non-urgent are done by medical professionals in the territory.
“We’ll always want individuals to be able to have the medical care that they need. Those determinations are made by their medical care providers in conjunction with radiologists that work on the MRI machine. Certainly, we know that a backlog of any patients waiting for even non-urgent care MRIs is not acceptable,” she said. “So we’re working to make sure that that changes.”
Contact Haley Ritchie at haley.ritchie@yukon-news.com