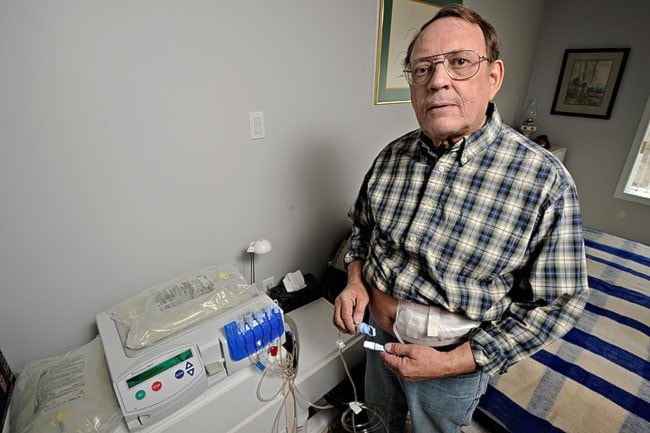
Michael Gladish wants to see better treatment for people with kidney disease in the Yukon.
He was diagnosed with the disease 12 years ago.
“The emotion that one goes through, and I’m not ashamed to admit it, is you have initial fear about the whole thing,” said Gladish, a Whitehorse resident. “Kidney failure is serious. You question your life, in the sense that you wonder, what did I do wrong? What could have caused the problem?”
Kidneys are responsible for pulling toxins out of the blood and out of the body through the urinary system.
When kidney failure becomes acute, the only options, besides waiting to die, are a transplant or dialysis.
The average wait for a transplant in Alberta is seven years, said Gladish.
He started dialysis treatment about half a year ago, and is hoping for a transplant in the next few years.
Here in the Yukon, no hospital-based dialysis treatment is available.
The B.C. Provincial Renal Agency delivers home-based treatment to Yukoners in need.
“The goal is to make it equitable no matter where you live,” said Dr. Adeera Levin, a nephrologist and the agency’s executive director.
Currently there are seven Yukon patients on peritoneal dialysis, and four on hemodialysis, according to the agency’s most recent statistics.
Peritoneal dialysis involves filling the abdomen with fluid through a surgically implanted catheter. Toxins move from the tissue into the fluid, which is then drained out through the same tube. The process needs special supplies but not necessarily any mechanical equipment or electricity.
With hemodialysis, the patient is hooked up to a large and complicated machine, and the blood itself is removed and cleaned before being returned to the body.
Whether a patient goes on peritoneal dialysis or hemodialysis is up to them, said Levin. Some people are medically better suited for one treatment over the other.
One of the great advantages of peritoneal dialysis is that it is transportable. A patient can take supplies with them and go anywhere in the world.
Gladish uses peritoneal dialysis. He has a suitcase-sized machine that automates the process of filling up his abdomen with fluid and draining it. He hooks himself into it before going to bed, and his blood is cleaned while he sleeps.
“Eventually you feel comfortable with your disease,” he said. “You begin to realize that you were really fortunate in the sense that you have support and you have good treatment and you have good doctors who care about what’s happening to you. Then you start to look at other people who have terminal illnesses like cancer and so forth and you realize how fortunate you are. You could be worse off.”
The good news for sufferers of kidney disease in the Yukon is that home-based therapies, the only kind available in territory, are in general better than hospital-based care.
A patient who goes to a renal clinic for hemodialysis would visit the centre three times a week for four hours each time. With home hemodialysis, they can hook up to the machine overnight every night of the week.
The home treatment offers both a higher level of blood-cleaning and a greater degree of independence for the patient, said Levin.
The problem for Yukon’s home hemodialysis patients is that if they get sick and have to visit the hospital, or if they are having trouble with their home therapy, they would have to leave the territory to receive hospital-based treatment.
But a full-blown renal clinic may not be the best solution, said Levin.
“The question is, do you need a big in-centre unit? Probably not. In fact, if we could turn the clock back, we wouldn’t have built all the in-centre units.”
A better solution would be to find a way to offer dialysis at the hospital not as regular, ongoing therapy but instead as interim therapy when home-based therapy is not possible.
“So instead of having to come all the way down to Vancouver, could we work out some kind of arrangement where there is the ability to do in-centre dialysis in Whitehorse for these specific kinds of things?” asked Levin. “That, to me, would be of value.”
There are few cases when home-based care is not possible, such as when a patient is severely crippled or mentally unwell, said Levin. But even then sometimes the patient’s home supports can make treatment possible.
“In a perfect world you would spend a lot more energy expanding home-based therapy, just because it’s better for people in general,” said Levin.
Before the conversation can start about what in-hospital dialysis would look like, the Yukon needs to assess the need for it, said Levin.
If all the patients can be treated at home, and might only need hospital treatments for short stints on an infrequent basis, it would be difficult and expensive to maintain the necessary resources.
“You would be training people and keeping their skills up for an occurrence that’s not very frequent,” said Levin.
But if demand increases, a conversation could start about how best to deliver those services.
“Could we work out some other clever system that would be more creative, that wouldn’t be as labour- or resource-intensive, perhaps? asked Levin.
In the meantime, the B.C. renal agency is developing innovative solutions like teleconferencing to give training to Yukon medical staff and give access to specialists to Yukon patients.
Early diagnosis and education can do much to improve outcomes for people with kidney disease, and in some cases ward off the need for dialysis altogether.
For that reason, Gladish urges Yukoners to make regular visits to their doctors.
“Kidney disease is a silent killer,” he said. “There are no tangible symptoms. You have no pain. You might go for years without even knowing that you have kidney disease, and the only way you ever find out - and this is how I found out - is by having a blood test, a simple blood test.”
Contact Jacqueline Ronson at
jronson@yukon-news.com